It would be quite silly of me to think the clinic here would function like my home hospital in Toledo; in fact, the whole reason I came here was to step outside my comfort level and see how austere medicine is practiced on the ground. Nothing, however, could have prepared me for what awaited my arrival at CEML.
Fighting through morning gridlock caused by lines at the petrol station, we meander through Lubango, up into the hills toward “Cristo Rei,” a replica of Christ the Redeemer in Rio de Janeiro. Three kilometers before the statue, we turn off onto a short dirt road which will deliver us to CEML. The grassy margin of the road is abustle with villagers waking from their slumber under trees and preparing meals over campfires. The clinic cannot afford to feed its inpatients, so families must travel with their loved ones to prepare their meals, feed them, and bath them. Often the portions heap in an almost comically mounded mass that seems impossible to consume in a single sitting. But consume they do, not for gluttony sake, however, quite the opposite. Patients and hospital staff often do not know when their next meal will come, so in times of plenty they pack in as much as they can in anticipation for times of scarcity.
The smell of the campfires follows us to the porticoed waiting area which is already full of new patients. Many traveled for days to get here and spent the night under the stars waiting for the gaggle of whitecoats to arrive in the morning. Though CEML is more a compound than a free-standing clinic, it is still quite small in comparison to the grand scale hospitals in town. Central Hospital, the Maternity Hospital, and the Children’s Hospital are all monolithic castles which loom over downtown Lubango like benevolent guardians. Unfortunately, nothing could be further from the truth. Relics of Angola’s ties to the communist empire, some facilities were built by China, others by Russia, and all are staffed by Cuban physicians who may, or may not, have wanted to come here. Infamous for refusing to integrate into Angolan culture, the Cubans speak a broken Span-uguese creole, take jobs from Angolan trained residents who go unemployed, and stopped developing their clinical thinking after medical school.
Often patients at these “hospitals” are victims of unspeakable horrors: surgeries by grossly unqualified practitioners, prescriptions of drugs with obvious interactions (or simply the wrong drugs for the condition), and an HIV department which only accepts 20 patients per day, so faculty can leave by 11am. Curiously, when these physicians leave, so too do the drugs used to treat HIV. Doctor Kubacki, the man who brought me to this country, comes to Lubango from his extremely remote clinic in Cavango once a month or so to procure meds. Outside the central pharmacy lurk the most unlikely drug dealers: men who speak in hushed tones offering quartan (malaria treatment), rifampin, or isoniazid (tuberculosis medications). Inside, the pharmacy is perennially short of supply (even when the drugs are clearly visible on the shelves). The pharmacists could be keeping the drugs for their own relations, for times of higher demand when they can raise prices, they may not want to give their drugs to the rural poor, or they could just not be in the mood to count pills.






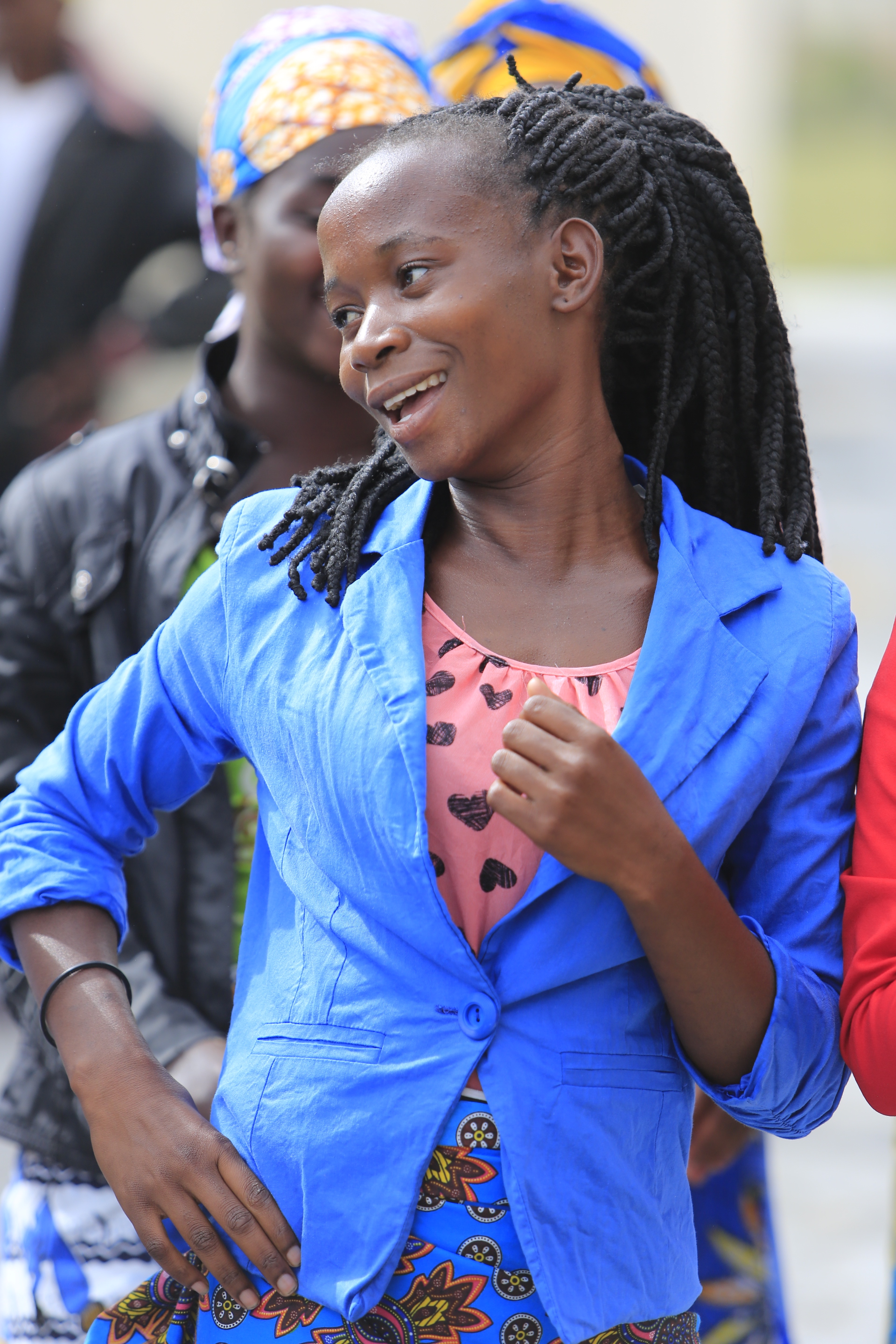



The Angolan government does not permit direct import of medical supplies from Namibia or the United States, which leaves clinicians precious few options to stock their shelves. Buying from the blackmarket scalpers outside the pharmacy will just perpetuate their fraud, so this is an absolute last resort. Local grocery store pharmacies must retire expired drugs, even though a military study of 20-year-old drugs found no loss of efficacy, or adverse effects, from all but aspirin or tetracycline respectively. Therefore, these expired meds are stockpiled by many physicians who practice in frontier clinics. But my favorite method? Smuggling. In a very “Robin Hood” reverse crime model, doctors have taken to road-tripping down to Namibia, buying drugs in bulk, and bootlegging them back across the border hidden within their 4x4s.
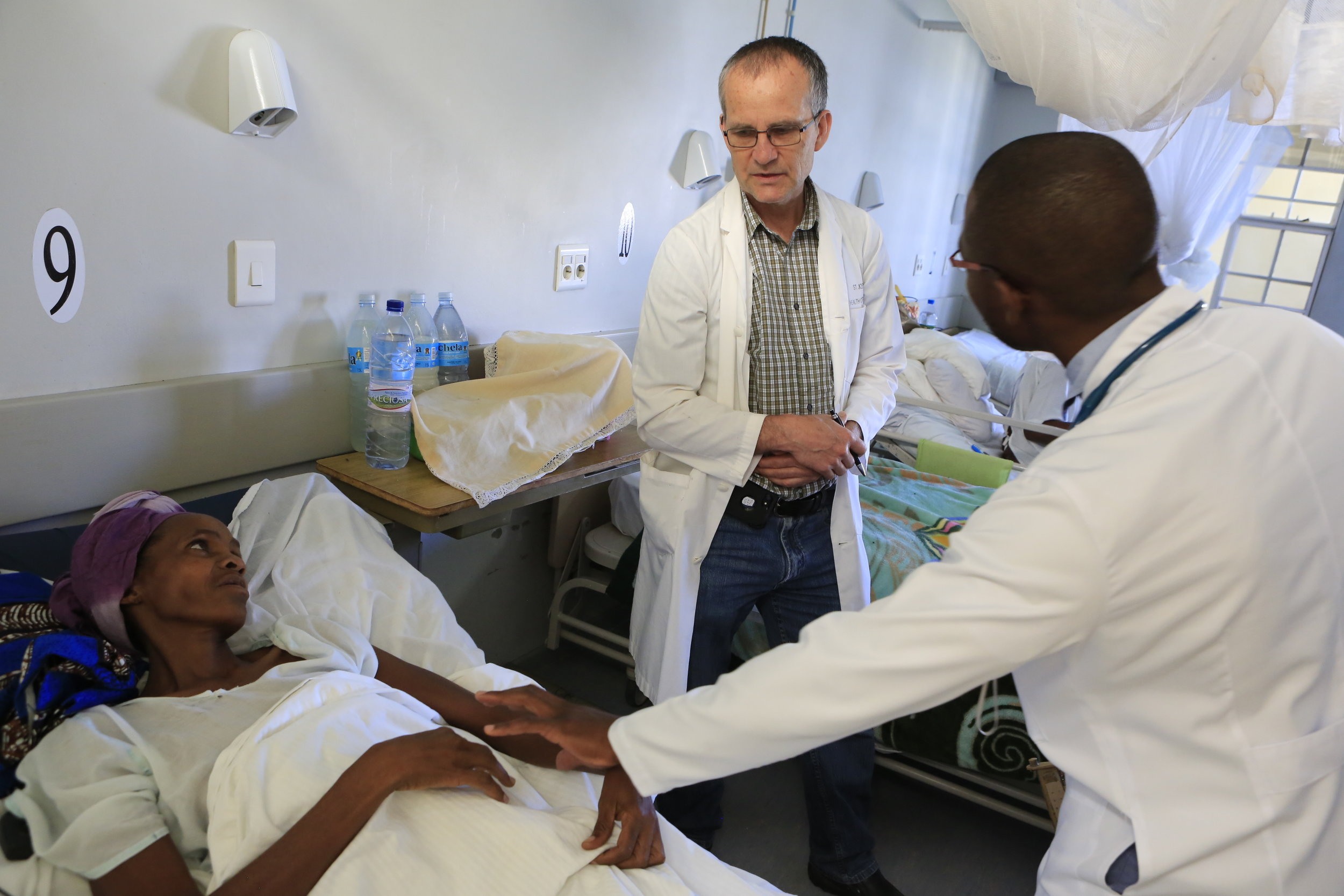
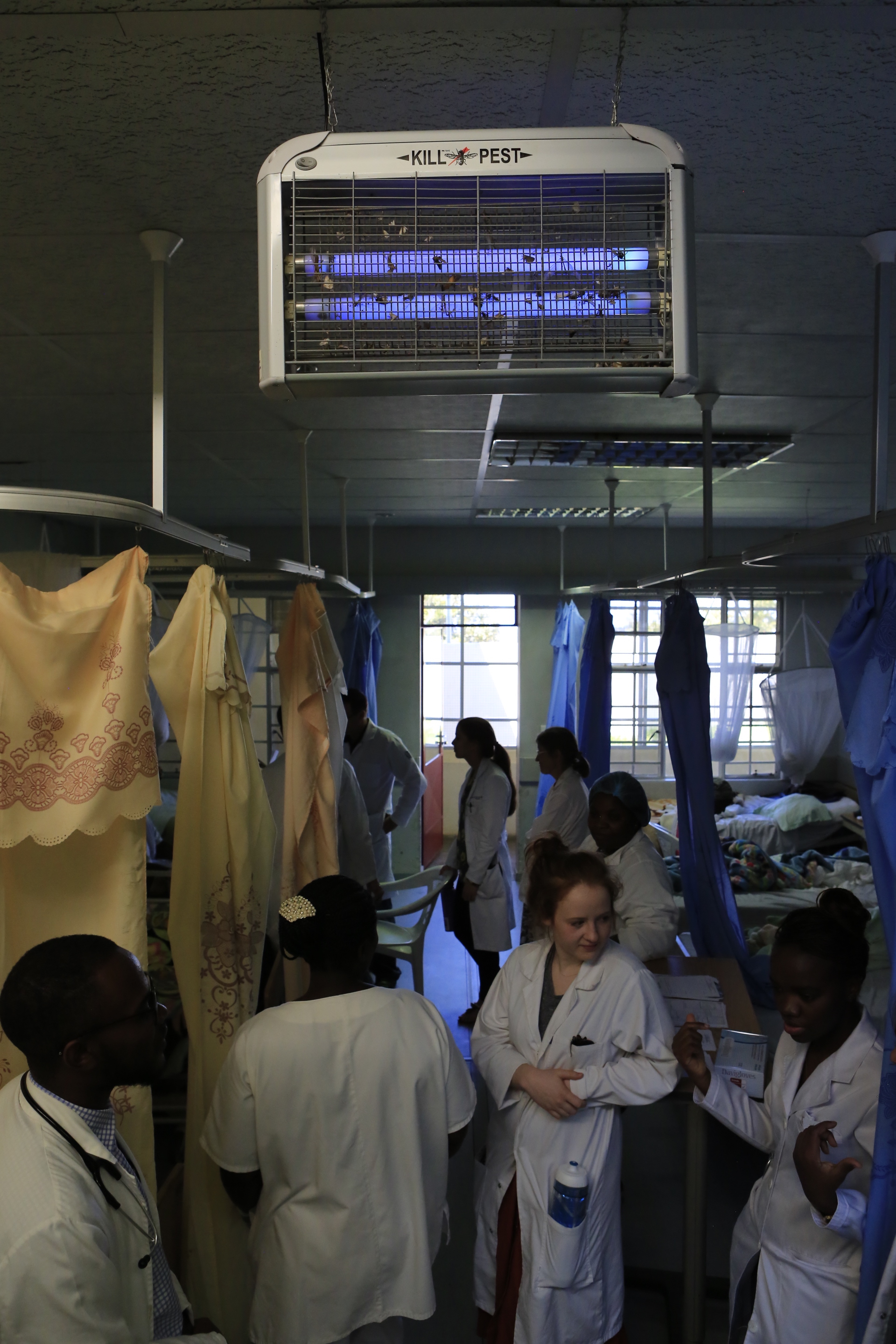
When the federal healthcare option offers poorly trained physicians, whose biggest concern is going home before lunch, and may or may not have access to medication, it’s easy to see why private clinics such as CEML are the preferred option. That does not mean to say we are the paragon of medical advancement. We do not have an x-ray, our lab is extremely limited, surgical instruments may have come from the hardware store (or be disposables that have been sanitized for reuse), scrub sponges that should be thrown away after one use are replaced weekly at best, and the pharmacy often stocks only one (often out-moded) drug from any given class. Anaesthesia for surgeries is similarly archaic with only local anaesthesia, or spinal block, in most cases (including open abdominal surgery). When this doesn’t take (or if the nurse missed the nerve), ketamine can put the patient in a dissociative state and help them forget the agony.
A common procedure here, in fact a specialty for which we are highly sought, is obstetric fistula repair. I knew coming here would expose me to things I could have never imagined, this is one of them. Nurse Audrey Henderson, my host-mother here in Lubango, directs the CEML fistula program and cares for all of the fistula women. She has gone so far as to develop a permanent encampment for the women just a hundred yards from the hospital, not only so they can receive immediate care if necessary, but so they can have their own sense of community and belonging. Audrey told me that the patients here are almost always abandoned by their “husbands,” a cruel practice that required explanation.
Obstetric fistulas happen when labor fails. In a developed nation we would rush a woman into the OR for a cesarean, but that is rarely available here; in a remote village, there is little that can be done. A witch doctor may concoct a tea with similar properties to oxytocin to promote further, harder contractions. The problem is rarely a lack of effort on the mother’s part, however, it is more likely to be incompatible anatomy (often because the mother is too young, and her hips too under-developed, to accommodate child birth). When the fetus is contracted against a birth canal which is physically incapable of expanding, delivery ceases, the fetus perishes, and the reproductive tissues are compressed so hard they cannot be perfused. Inevitably this causes tissue death, necrosis, and the formation of a fistula (a non-anatomic hole which opens between the vagina and either the bladder, rectum, or both).
Not only does the poor mother then smell of rotting flesh, but she is now incontinent of stool and urine and truly cannot stay clean. Even if a husband could cope with this, his young wife is also now infertile and will not bare him any children; for most this is too much to take and they will leave to find a new bride. Rejected and alone, these women find new hope after receiving a surgical closure of their fistulas and in Audrey’s special patient village. In fact, they celebrate and sing together, casting off the darkness of their old lives, and accepting a new life together. They invited Dr. Haniel and I as special male guests; I’m glad he was there to translate for me or I would have been lost.
I guess I’m gonna have to pick up some Portuguese. Let’s start simple with the traditional Angolan greeting: dormiste bem?

